Symptoms of ILD
Although interstitial lung diseases may have different causes and features on CT scan and on biopsy, and even different treatments, they share many of the same symptoms.
- No symptoms: Some people are very surprised that they have a serious lung disease because they feel no symptoms. Perhaps their ILD was noticed on a chest x-ray or CT that they got for work or during a surgical workup.
- Shortness of breath (dyspnea): Many people notice shortness of breath, also called dyspnea, especially while going up hills or stairs. Many people think it’s just old age and do not seek advice for their short
- Fatigue: Many people report that they become fatigued easily, especially with activity. Again, many people think it’s just because of old age.
- Dry, hacking cough: Many people have a persistent dry cough that produces little or no phlegm. Some cough whenever they talk, others cough only at night or only in the morning. Some cough all the time and report that it’s their most annoying symptom.
Managing symptoms in ILD is very important in the overall management of interstitial lung disease. See Symptom Management section for further information about symptom management in ILD.
How is ILD diagnosed?
Remember that there are many interstitial lung diseases. It is important to get an accurate ILD diagnosis so that you can get the right treatment. The diagnosis of interstitial lung disease requires a team of providers working together to review tests. There are several tests and tools commonly performed for diagnosing interstitial lung.
In making a diagnosis, your provider will start by conducting a thorough medical history and physical examination. This will include discussing your health history, reviewing medications and potential occupational and environmental exposures, listening to your chest with a stethoscope to check for a crackling sound and carefully examining your skin and joints. They might suggest you get lab tests and/or to be referred to other specialists who can help weigh in on the most likely diagnosis.
History and Physical Exam
The history and physical is the most important tool used in diagnosing interstitial lung disease and comorbidities. Your provider will ask you many questions, some of which might seem strange to you and unrelated to your lungs. S/he will also perform a physical exam, which would include not only your lungs, but also your skin, fingernails, and joints. Some examples of questions you may be asked are:
- Medical history
- Family history
- Medications
- Many questions about possible environmental and occupational exposures
Pulmonary Function Tests (PFTs)
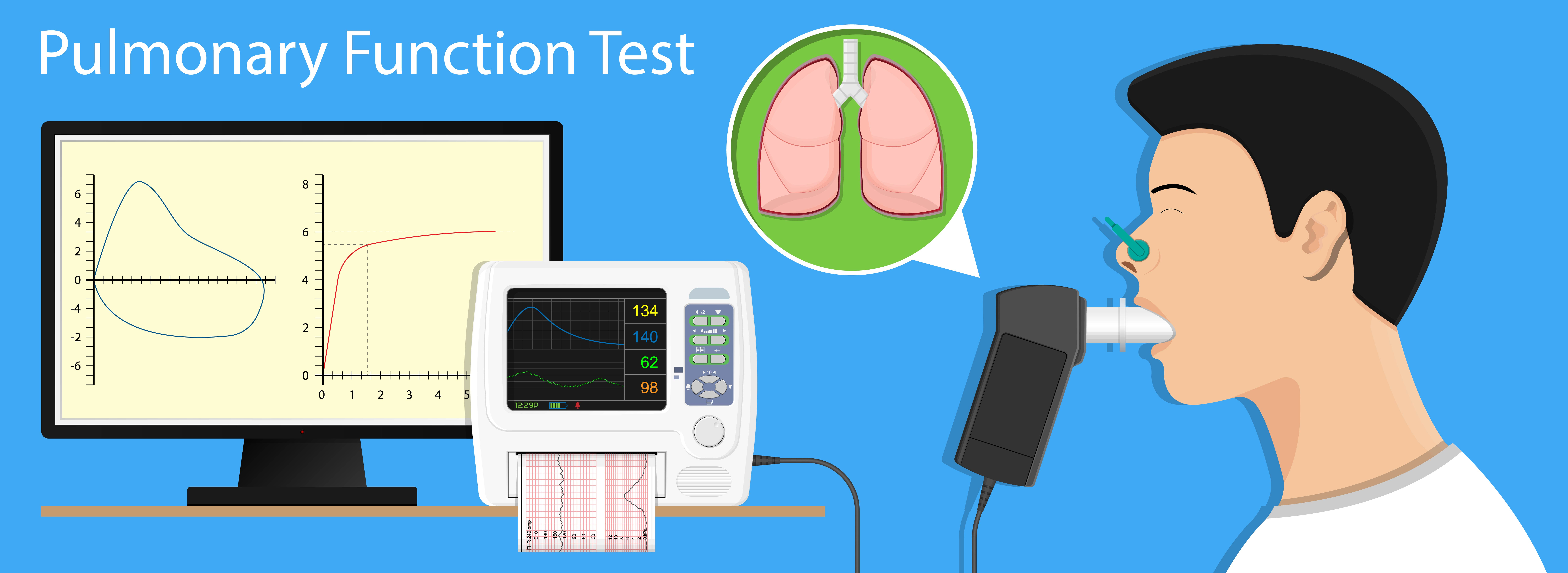
These are tests of various aspects of your lung function, such as how much air your lungs can hold, how well air moves in and out of your lungs, and the ability of oxygen to get into your bloodstream. Pulmonary function tests are often performed by primary care providers or pulmonologists in their offices. Full pulmonary function tests can take up to an hour to perform, and may be done in your provider’s office or even in a pulmonary function lab in a hospital. These tests are very useful in diagnosing interstitial lung disease. They are also used to monitor you over time. You may be asked to repeat PFTs every 3 - 6 months, so that your provider can tell how your lungs are doing.
You can go here for a good description of pulmonary function tests.
High Resolution Computerized Tomography or High Resolution CT scan (HRCT)
This scan is critical for determining what type of interstitial lung disease you have. A high resolution CT scan shows more details than a regular CT scan. The HRCT scan usually takes less than half an hour. You will be asked to lie on a table. A large, doughnut-shaped machine will move around you and take pictures of your lungs. The pictures are converted into digital images and copied onto a CD. Unlike an MRI, there is no enclosed chamber involved in HRCT scanning.
You can find UCSF’s protocol for high resolution CT scanning of the chest by clicking here.
NOTE: You may be asked to repeat PFTs and HRCT scans at regular intervals to follow the course of your disease. Watching the results of these two tests over time helps your doctor determine whether your disease is progressing, or how well a medication is working.
Blood tests
Several types of blood tests are used to diagnose interstitial lung diseases.
- Serologies to look for certain antibodies in the blood that might identify a connective tissue disorder, such as rheumatoid arthritis or scleroderma, as the cause of the ILD. Serologies might include blood tests like RF, ANA, CPK, CCP, aldolase, SSA, SSB, SCL-70 Jo-1 and more. Even if you’ve had serologies drawn in the past, your provider may want to repeat them.
- Blood markers to identify gene mutations. These are often performed when it is suspected that an interstitial lung disease runs in a family, or when a person’s ILD has features of a genetic disorder.
Please go to the section on "Familial Pulmonary Fibrosis, Telomeres, and Genetic Testing" in Resources to learn more about genetic testing in ILD.
Bronchoscopy
This procedure is used to diagnose some types of interstitial lung diseases. For a bronchoscopy, you are awake but sedated by medication that is is administered intravenously, so you are comfortable and often do not feel or remember the procedure. It is performed by a pulmonologist, usually in a special room in the hospital. A flexible tube that’s about the diameter of a pencil is carefully passed into the airways of your lungs through your mouth or nose. There is a light, camera, and tiny instruments in the tube, so the doctor can examine your airways, take tiny pieces of lung tissue (a “transbronchial biopsy”), or collect cells by “washing” them out with a salt water solution. The tissue and cells are then analyzed to help with diagnosis. After a bronchoscopy, you will stay in a hospital bed for a few hours, then, if there are no problems, you will be able to go home. You will be asked to have a friend or family member drive you home after the procedure. You may have a sore throat, cough, or hoarseness for a few days. Your doctor will decide if this is the right procedure for you.
Video-Assisted Thorascopic Surgery (VATS biopsy)
If your doctor cannot make a diagnosis from the HRCT scan and a bronchoscopy, s/he may ask you to undergo a surgical lung biopsy, in order to get a large enough lung tissue sample for proper diagnosis. VATS biopsy is performed by a chest (thoracic) surgeon in the hospital and involves at least a one night stay, sometimes more. Surgical lung biopsy provides your pulmonologist with a larger sample of lung tissue from several different areas of your lung. Please see VATS Biopsy in the “Learn More” section for a full description of this procedure.
Multi-disciplinary case conference

ILDs can be complex and difficult to diagnose. Nevertheless, an accurate diagnosis is critical, because treatment and prognosis differ among the interstitial lung diseases. A multidisciplinary case conference is an important tool in the diagnosis of ILD. It assures that the ILD pulmonologist (along with any other discipline that is relevant to the diagnosis in question, such a rheumatologist), radiologist, and pathologist sit down together to review and discuss a patient’s history, physical, and test results. Because ILDs can be difficult to diagnosis, and because it has been shown that a multidisciplinary case conference can improve the accuracy of ILD diagnosis, the multi-disciplinary case conference has become standard of care for diagnosing ILD.
